
Cedarhurst (516) 374-3668
Franklin Square (516) 775-8440

Cedarhurst (516) 374-3668
Franklin Square (516) 775-8440
When the heart pumps blood around the body, it is called circulation. Good blood circulation works to provide oxygen and nutrients to cells and remove waste from the body. Factors that can lead to poor circulation include high or low blood pressure, high red blood cells, a weak heart, and problems with veins and arteries interfering with the flow of blood to the body. Circulation can be improved by being more active, implementing cardiovascular and stretching exercises, and maintaining good health habits, like having a healthy body weight and not smoking. Other ways include reducing saturated fats, increasing omega-3 fatty acids and antioxidants in the diet, and having a balanced level of iron intake. Underlying conditions that can impact proper blood circulation include obesity, diabetes, and a heart condition. When one has poor circulation they may experience numbness, tingling, and pain in their limbs, including the feet. This can lead to falls or other conditions that can be dangerous and should be checked by a qualified podiatrist who can examine the feet, diagnose problems, and suggest proper treatment methods.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact Robert Stein, DPM of South Shore Foot Care. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact our offices located in Cedarhurst and Franklin Square, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
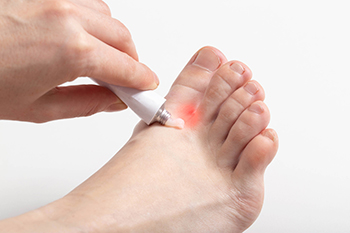 The most common type of athlete’s foot is referred to as chronic interdigital. Symptoms that are associated with this condition often include itchiness between the toes and on the bottom of the foot. It can develop as a result of wearing shoes that are too small, and this can create a warm environment that is perfect for fungus to grow in. The least common type of athlete’s foot is known as vesicular, and this can produce blisters that are painful on the bottom or top of the foot. Athlete’s foot is contagious and may be prevented by wearing appropriate shoes in public showers. If you have developed this uncomfortable foot condition, it is strongly suggested that you consult with a podiatrist who can begin the correct treatment for you.
The most common type of athlete’s foot is referred to as chronic interdigital. Symptoms that are associated with this condition often include itchiness between the toes and on the bottom of the foot. It can develop as a result of wearing shoes that are too small, and this can create a warm environment that is perfect for fungus to grow in. The least common type of athlete’s foot is known as vesicular, and this can produce blisters that are painful on the bottom or top of the foot. Athlete’s foot is contagious and may be prevented by wearing appropriate shoes in public showers. If you have developed this uncomfortable foot condition, it is strongly suggested that you consult with a podiatrist who can begin the correct treatment for you.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Robert Stein, DPM from South Shore Foot Care. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our offices located in Cedarhurst and Franklin Square, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
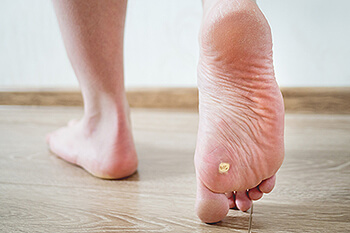 If you have a small growth or lesion near the base of your toes or bottom of the heel, you may have developed a plantar wart. Plantar warts are caused by HPV (human papillomavirus) which enters the foot through cuts or breaks in the skin on the bottom of the feet. These warts can grow beneath a callus on the foot if enough pressure is put on them. They can also cause pain or tenderness when standing or walking. Plantar warts are not particularly serious and may even go away on their own, but they can also remain, come back, or multiply. If you have a plantar wart, it is suggested that a qualified podiatrist examine your foot to verify the growth as well as provide treatments that increase your comfort.
If you have a small growth or lesion near the base of your toes or bottom of the heel, you may have developed a plantar wart. Plantar warts are caused by HPV (human papillomavirus) which enters the foot through cuts or breaks in the skin on the bottom of the feet. These warts can grow beneath a callus on the foot if enough pressure is put on them. They can also cause pain or tenderness when standing or walking. Plantar warts are not particularly serious and may even go away on their own, but they can also remain, come back, or multiply. If you have a plantar wart, it is suggested that a qualified podiatrist examine your foot to verify the growth as well as provide treatments that increase your comfort.
Plantar warts can be very uncomfortable. If you need your feet checked, contact Robert Stein, DPM from South Shore Foot Care. Our doctor will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
Treatment
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions, please feel free to contact our offices located in Cedarhurst and Franklin Square, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Heel pain is a very common occurrence. It is usually felt under the heel or at the back of the heel. When pain and inflammation is located on the bottom of the heel toward the front of the foot, plantar fasciitis is typically the cause. Plantar fasciitis is a painful inflammation of the plantar fascia tissue, which runs along the bottom of the foot and connects the heel with the toes. Other causes of heel pain on the bottom of the foot may be attributed to heel pad atrophy or heel spurs. If pain is felt at the back of the heel, Achilles tendonitis is often at the root of the cause. This condition occurs when the Achilles tendon, which attaches to the back of the heel bone, becomes damaged or torn over time, causing pain and swelling. Other possible causes include bursitis, Sever’s disease, and heel bumps. Pain from a heel stress fracture can occur anywhere on the heel, and tarsal tunnel syndrome can cause heel pain underneath the ankle bone. Heel pain can also be caused by neurological issues, infections and arthritis. Unless you suffer an acute injury, heel pain typically starts out mild, but can become severe. If you are experiencing any type of heel pain, don’t hesitate to contact a podiatrist to find out the cause and take measures to keep it from worsening or becoming chronic or debilitating.
Many people suffer from bouts of heel pain. For more information, contact Robert Stein, DPM of South Shore Foot Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Cedarhurst and Franklin Square, NY . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Every patient is unique and so are treatments. The information on this website is for educational purposes and each individual
patient care model may differ.